Mammography (Breast X-ray)
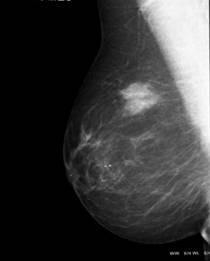 Mammography is a way of imaging the breast tissue and produces an X-ray called a mammogram. The breast is ‘squashed’ between two plastic plates while a beam of X-rays passes through the breast tissue and on to an X-ray film. This ‘squashing’ of the breast may be a little uncomfortable, but it only lasts for approximately 30 seconds. The radiation doses used during mammography are much too small to be significant in causing cancer.
Mammography is a way of imaging the breast tissue and produces an X-ray called a mammogram. The breast is ‘squashed’ between two plastic plates while a beam of X-rays passes through the breast tissue and on to an X-ray film. This ‘squashing’ of the breast may be a little uncomfortable, but it only lasts for approximately 30 seconds. The radiation doses used during mammography are much too small to be significant in causing cancer.
The mammogram appears as a mixture of white, grey and black shadows that can be interpreted by a specialist doctor, called a radiologist. Mammograms are 85% accurate in the diagnosis of breast cancer.
Scientific studies in western Europe have shown that breast cancer screening with mammography has reduced the number of deaths from breast cancer by approximately 30%. This applies only to women aged over 50 years, because mammograms are less likely to show cancers in younger women (with dense breasts). Breast cancers detected by screening are usually at an early stage or are non-invasive cancers that can be treated more effectively.
Screening programmes in countries such as the UK offer mammography to women aged 50-65 years once every three years. It is now believed this is too long an interval to go between breast screens, and it is the author’s opinion that women aged between 50 and 69 years should have a mammogram every 1 to 2 years and that women aged 40-49 years should be screened by digital mammography every year. Digital mammography is more accurate that analogue mammography in breast cancer detection esp. in premenopausal women and those taking HRT. Furthermore it allows the use of a lowe radiation dose.
For more information on this topic : http://www.issoonline.com/content/3/1/4
Women with a strong family history of breast cancer are advised to have screening digital mammography from the age of 35 years. As mentioned earlier, younger women (below 35 years) tend to have denser breasts and, therefore, the mammogram may not show any abnormal shadows as clearly as in older women. Current research is trying to find better methods of screening younger women, such as magnetic resonance imaging (MRI) and ultrasound scan. Recent evidence strongly suggests that MRI is the best method of screening high-risk younger women.
What Happens if I Have an Abnormal Mammogram?
If the mammogram does show an indeterminate abnormality, the woman will be recalled to the clinic and examined by a breast specialist. Further tests may be required; these include a needle biopsy of the breast and/or an ultrasound scan.
The tests may reveal that there is a breast lump corresponding to the abnormal shadow on the mammogram. Occasionally, no further tests will be required and the patient will be advised to have a follow-up mammogram in a year, or to continue in the screening programme. If the biopsy shows that cancer cells are present, the patient is treated accordingly. Indeterminate microcalafications (white spots) are assessed with vaccuum biopsy under imaging guidance.
Professor Mokbel endorses The American College of Radioloy and Society of Breast Imaging guidelines of annual screening mammography from the age of 40 for women at an average risk of the disease.
https://jamanetwork.com/journals/jama/fullarticle/2463262
For detailed information regarding the benefits and harms of breast cancer screening
https://jamanetwork.com/journals/jama/fullarticle/2463261

